Table of Contents
Introduction:
Paroxysmal supraventricular tachycardia (PSVT) is one of the most common forms of cardiac arrhythmia encountered in clinical practice. It is characterized by sudden episodes of abnormally fast heart rate that begin and end abruptly. These episodes can cause palpitations, dizziness, chest discomfort, shortness of breath, and anxiety, often sending patients to emergency departments repeatedly.
The approval of etripamil has marked a major advancement in the management of PSVT. Etripamil is a novel, self-administered intranasal medication designed for rapid termination of acute PSVT episodes. At the heart of its clinical success lies the etripamil mechanism of action, which precisely targets the electrical pathways responsible for abnormal heart rhythms.
Understanding the etripamil mechanism of action is essential for clinicians, pharmacists, students, and patients because it explains how the drug restores normal heart rhythm quickly, why it acts faster than many traditional therapies, and why it is safer for outpatient use. This detailed article explores the pharmacology, clinical relevance, FDA approval, side effects, drug interactions, and real-world implications of etripamil in a comprehensive, easy-to-understand manner.
Overview of Etripamil: A New-Generation Antiarrhythmic Drug
Etripamil is a short-acting, non-dihydropyridine calcium channel blocker developed specifically for the acute treatment of PSVT. Unlike conventional antiarrhythmic medications that require intravenous administration in a hospital setting, etripamil is delivered via a nasal spray, allowing patients to treat episodes at home or wherever symptoms occur.
The drug is designed for on-demand use, not daily maintenance therapy. This approach is revolutionary because PSVT episodes are intermittent and unpredictable. The unique design and pharmacological profile of etripamil align perfectly with this need, and the etripamil mechanism of action is central to this innovation.
Understanding PSVT: The Condition Etripamil Treats
Before diving deeper into the etripamil mechanism of action, it is important to understand PSVT itself.
What Happens in PSVT?
PSVT occurs when abnormal electrical circuits form in the atria or around the atrioventricular (AV) node. These circuits allow electrical impulses to loop repeatedly, causing the heart to beat rapidly — often between 150 and 250 beats per minute.
Key characteristics include:
- Sudden onset and termination
- Rapid, regular heart rhythm
- Dependence on AV nodal conduction
Because the AV node plays a central role in PSVT, it becomes the primary pharmacological target — and this is exactly where the etripamil mechanism of action exerts its effects.
Core Concept: Etripamil Mechanism of Action Explained
The etripamil mechanism of action involves selective inhibition of L-type calcium channels in cardiac tissue, particularly within the atrioventricular node.
Role of Calcium Channels in Cardiac Conduction
Calcium ions are essential for:
- Electrical signal propagation in nodal tissue
- Cardiac muscle contraction
- Regulation of heart rhythm
In the AV node, calcium currents determine how fast electrical impulses pass from the atria to the ventricles. Excessive calcium influx supports re-entrant circuits that sustain PSVT.
Step-by-Step Breakdown of the Etripamil Mechanism of Action
The etripamil mechanism of action can be understood through the following sequence:
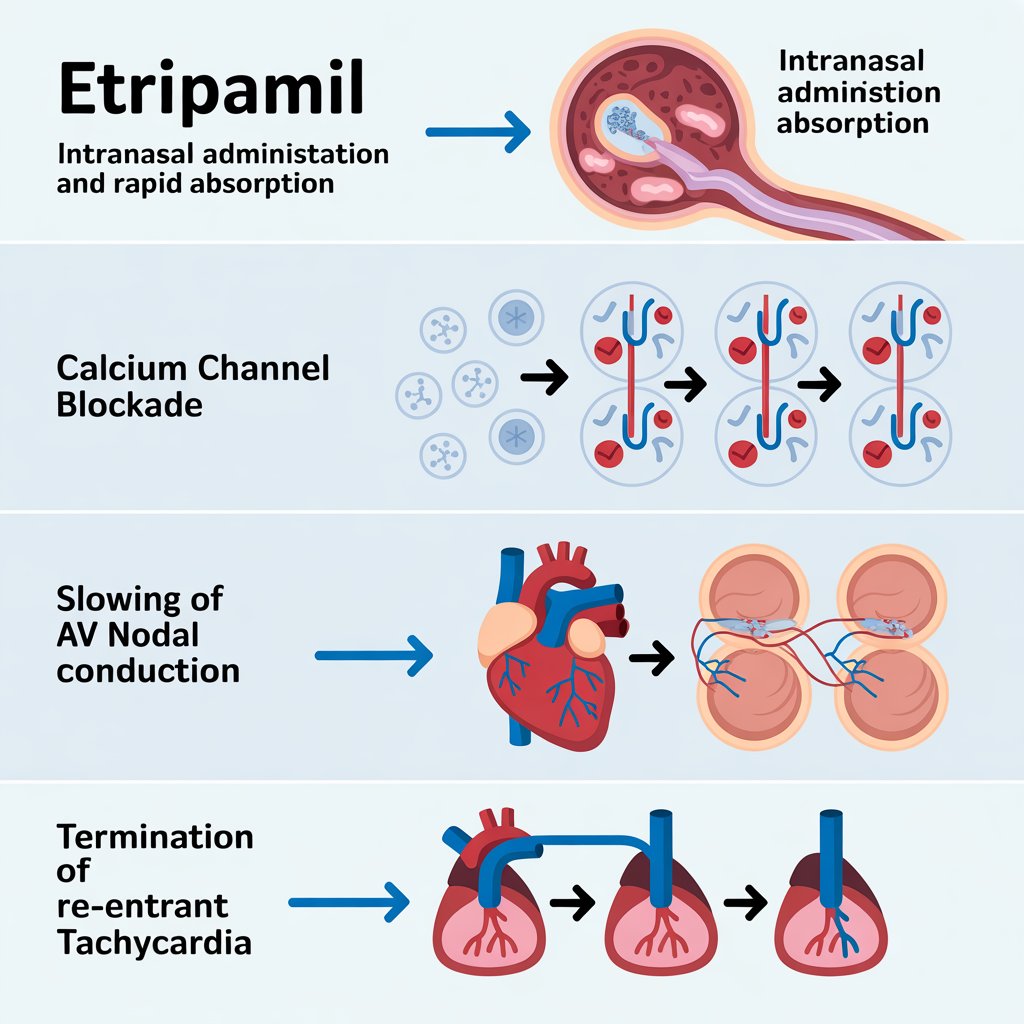
1. Intranasal Administration and Rapid Absorption
Etripamil is administered as a nasal spray. The nasal mucosa is highly vascularized, allowing the drug to enter systemic circulation rapidly without first-pass hepatic metabolism.
This fast absorption ensures that the etripamil mechanism of action begins within minutes of administration.
2. Calcium Channel Blockade
Once absorbed, etripamil binds to L-type calcium channels located on cardiac myocytes and nodal cells. By blocking these channels, etripamil reduces the influx of calcium ions during the cardiac action potential.
This calcium channel blockade is the foundation of the etripamil mechanism of action.
3. Slowing of AV Nodal Conduction
By reducing calcium entry:
- AV nodal conduction velocity decreases
- The refractory period of the AV node increases
- Electrical impulses are temporarily blocked or delayed
This disruption halts the re-entrant electrical loops responsible for PSVT.
4. Termination of Re-entrant Tachycardia
As conduction through the AV node slows sufficiently, the abnormal circuit collapses. Normal sinus rhythm is restored, often within 10–30 minutes.
This precise targeting explains why the etripamil mechanism of action is both effective and predictable.
Why the Etripamil Mechanism of Action Is Unique
The etripamil mechanism of action differs from other calcium channel blockers in several critical ways:
- Ultra-short duration: Effects wear off relatively quickly
- Minimal systemic accumulation
- Reduced risk of prolonged hypotension
- Designed for acute, not chronic, use
These properties make etripamil particularly suitable for outpatient self-administration.
Pharmacodynamics: Functional Effects of Etripamil on the Heart
Pharmacodynamics refers to what the drug does to the body. The etripamil mechanism of action leads to measurable changes in cardiac electrophysiology.
Electrocardiographic Effects
- Temporary prolongation of the PR interval
- No significant QT prolongation
- Minimal effect on ventricular conduction
These changes reflect slowed AV nodal conduction — the intended therapeutic effect.
Hemodynamic Effects
Because etripamil is short-acting:
- Blood pressure reductions are generally mild and transient
- Cardiac output is preserved
- Reflex tachycardia is uncommon
This safety profile is directly linked to the controlled nature of the etripamil mechanism of action.
Pharmacokinetics Supporting the Mechanism of Action
The success of the etripamil mechanism of action depends on its favorable pharmacokinetics.
Absorption
- Rapid nasal absorption
- Onset of action within minutes
Distribution
- Moderate protein binding
- Efficient cardiac tissue penetration
Metabolism
- Metabolized by esterases and hepatic enzymes
- Minimal accumulation with single-dose use
Elimination
- Short plasma half-life
- Rapid decline in systemic exposure
Together, these properties ensure that the etripamil mechanism of action is fast, effective, and self-limiting.
FDA Approval and Regulatory Milestones
Etripamil received FDA approval for the acute treatment of PSVT in adults after extensive clinical evaluation.
Why FDA Approval Was Significant
- First intranasal antiarrhythmic drug
- First self-administered therapy for PSVT
- Reduced reliance on emergency care
The FDA approval validated both the safety and effectiveness of the etripamil mechanism of action in real-world patients.
Clinical Trial Outcomes
Clinical studies demonstrated that:
- Etripamil converted PSVT to sinus rhythm significantly faster than placebo
- Symptom relief occurred rapidly
- Many patients avoided emergency department visits
These outcomes confirm that the etripamil mechanism of action translates directly into clinical benefit.
Side Effects of Etripamil
Understanding side effects is essential when discussing the etripamil mechanism of action.
Common Side Effects
Most adverse effects are mild and localized:
- Nasal irritation
- Nasal congestion
- Runny nose
- Mild nosebleeds
These effects are related to nasal administration rather than systemic toxicity.
Cardiac-Related Side Effects
Due to its action on AV nodal conduction:
- Temporary slowing of heart rate
- Transient PR interval prolongation
- Rare cases of short-lasting AV block
These effects are predictable consequences of the etripamil mechanism of action.
Serious Adverse Effects (Rare)
- Severe hypotension
- High-grade AV block
- Syncope
Such events are uncommon and typically associated with pre-existing cardiac conditions.
Drug Interactions and Clinical Considerations
The etripamil mechanism of action can be influenced by other medications.
Potential Drug Interactions
- Other calcium channel blockers
- Beta-blockers
- Antiarrhythmic agents
- CYP3A4 inhibitors or inducers
Combined use may increase the risk of excessive AV nodal suppression.
Precautions
Caution is advised in patients with:
- Severe hypotension
- Advanced AV block
- Structural heart disease
Understanding these risks helps optimize the safe use of the etripamil mechanism of action.
Contraindications
Etripamil should generally be avoided in patients with:
- Second- or third-degree AV block without pacemaker
- Severe bradycardia
- Known hypersensitivity to calcium channel blockers
Patient Education and Practical Use
Patients prescribed etripamil should be educated on:
- Proper nasal spray technique
- Recognizing PSVT symptoms
- When to seek emergency care
Clear patient education enhances the effectiveness of the etripamil mechanism of action in real-world use.
Advantages of Etripamil Over Traditional Therapies
Compared with intravenous antiarrhythmics:
- No need for hospital access
- Faster patient-controlled treatment
- Reduced healthcare burden
These advantages stem directly from the optimized etripamil mechanism of action.
Future Potential of Etripamil
Research is ongoing to explore:
- Broader arrhythmia indications
- Improved formulations
- Combination therapy strategies
The unique etripamil mechanism of action positions it as a model for future acute-use cardiovascular drugs.
Conclusion: The Clinical Importance of the Etripamil Mechanism of Action
The etripamil mechanism of action represents a major innovation in cardiac pharmacotherapy. By selectively blocking L-type calcium channels in the AV node, etripamil rapidly interrupts re-entrant electrical circuits responsible for PSVT while minimizing systemic exposure.
Its fast onset, short duration, nasal delivery, and patient-controlled use make it a landmark therapy in arrhythmia management. As clinical adoption grows, a clear understanding of the etripamil mechanism of action will remain essential for safe, effective, and confident use by healthcare professionals and patients alike.

