Table of Contents
Epcoritamab – an advanced immunotherapy used in certain B-cell lymphomas – offers hope to many patients. But like many powerful treatments, it has a spectrum of side effects. Fully understanding the Epcoritamab Side Effects can help patients and caregivers stay informed, respond promptly to concerns, and increase safety while getting the most out of therapy.
In this guide, we explore common and mild reactions as well as serious and potentially life-threatening reactions. We also cover when Epcoritamab Side Effects occur, why they occur, how to manage them, and when to seek immediate medical attention. Finally, we provide practical advice for patients and caregivers to navigate treatment with confidence.
Important: This content is for informational purposes only. Always follow the guidance of your treating oncologist or hematologist. If you experience any troubling symptoms, contact your care team immediately.
What Is Epcoritamab and Why Epcoritamab Side Effects Occur
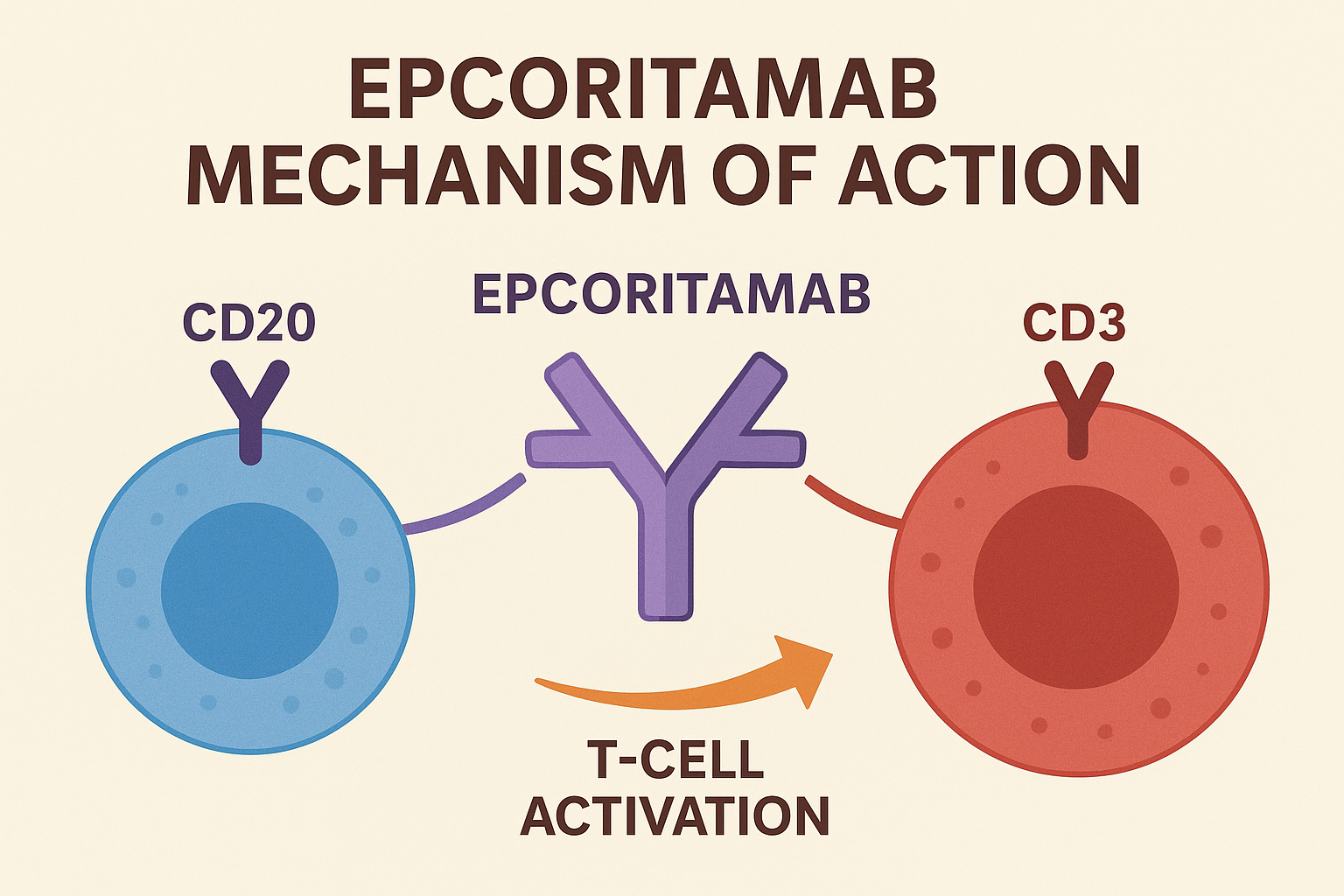
Epcoritamab is not a traditional chemotherapy – it works by using the body’s own immune system. Specifically:
• It binds to CD20 on malignant B-cells (as well as healthy B-cells).
• At the same time, it binds to CD3 on T-cells, redirecting T-cells to attack those CD20-positive B-cells.
This immune-mediated mechanism can lead to strong anti-cancer effects – but also initiates immune activation, which can lead to a variety of Epcoritamab Side Effects . Some reflect overactivation of the immune system (e.g., inflammation, fever), others reflect suppression or collateral damage (e.g., reduction in blood cells), and some arise from how the drug is given (e.g., injection-site reactions).
Due to this dual nature – powerful therapy + immune involvement – side effects are an expected part of treatment with Epcoritamab.
Common / Mild to Moderate Epcoritamab Side Effects
Many patients receiving Epcoritamab side effects that are manageable, especially with appropriate supportive care. Below are frequently reported issues:
Fatigue and General Weakness
- Feeling unusually tired or lethargic, even after rest.
- Need for longer periods of rest or sleep, reduced motivation, or difficulty engaging in daily activities.
- In some cases, fatigue may persist for a few days after a dose, then gradually improve.
Muscle, Joint, or Bone Discomfort
- Aching muscles, joint stiffness, or generalized bone/muscle pain.
- Sometimes described as “flu-like” aches, or soreness after injection.
- Often manageable with rest, gentle movement, hydration, and — if allowed by the care team — mild pain relief.
Injection-Site Reactions (for Subcutaneous Administration)
Because it is administered under the skin it shows Epcoritamab Side Effects :
- Redness, swelling, warmth, itching, or tenderness at the injection site.
- Mild bruising or small local bruises.
- These reactions are usually local and self-limiting, resolving over a few days.
Gastrointestinal Symptoms
Many patients may experience following Epcoritamab Side Effects:
- Nausea or mild queasiness.
- Decreased appetite, or temporary loss of interest in food.
- Abdominal discomfort, mild cramping, diarrhea or constipation (less common).
- These symptoms may worsen shortly after a dose, but often subside with time and supportive care (e.g., hydration, light meals, anti-nausea medication if prescribed).
Mild Flu-like Symptoms, Fever, or Infections
Because immune activation — or transient immune suppression — can occur, some patients report:
- Low-grade fever, chills, or general “feeling unwell.”
- Mild upper respiratory symptoms (e.g., sore throat, mild cough), or mild infections that resolve without major complications.
- Slower healing of minor wounds, or increased susceptibility to common infections (like colds) — especially if blood counts drop.
Headache, Dizziness, or Light-headedness
Some patients may feel because of Epcoritamab Side Effects:
- Headaches of mild to moderate intensity.
- Light-headedness or episodes of mild dizziness, particularly shortly after infusion or injection.
- These symptoms tend to be transient — often resolving on their own — but should be reported if persistent or worsening.
Serious or Potentially Dangerous Epcoritamab Side Effects
While many Epcoritamab Side Effects are manageable, certain adverse reactions associated with Epcoritamab require urgent attention. These are less common, but potentially life-threatening. Understanding them is vital for safe therapy.
Cytokine Release Syndrome (CRS) — Immune Overreaction
What is CRS?
CRS arises when immune activation triggered by Epcoritamab leads to a massive release of inflammatory cytokines — chemical messengers — resulting in systemic inflammation. Because Epcoritamab mobilizes T-cells against B-cells, immune cells suddenly become very active; in some patients, this causes a widespread “immune storm.”
Typical signs and symptoms of CRS may include:
- High fever, chills, shivers
- Rapid heartbeat (palpitations, tachycardia)
- Rapid or difficult breathing, shortness of breath
- Low blood pressure, dizziness, fainting, or light-headedness
- Nausea or vomiting
- Severe fatigue, weakness, or malaise
- Muscle or joint pains, body aches — similar to a harsh flu
- Headache, sometimes severe
When does CRS usually occur?
- Most commonly during the first few doses — especially the first full therapeutic dose.
- Because of this, many treatment protocols include careful monitoring under hospitalization or supervised setting during early doses.
- However, CRS may also arise after later doses, albeit less commonly.
Why CRS matters:
If CRS becomes severe and uncontrolled, it can affect vital organs (heart, lungs, kidneys), lead to dangerously low blood pressure, breathing difficulties — potentially life-threatening without prompt care.
Neurotoxicity / Neurologic Epcoritamab Side Effects (Immune-Mediated)
Because Epcoritamab modulates the immune system, in some cases the immune activation — or its byproducts — can also affect the central nervous system. Possible neurologic or neurotoxic Epcoritamab Side Effects can include:
- Confusion, disorientation, or altered mental status
- Difficulty in speaking clearly, slurred speech, trouble finding words
- Tremors, uncoordinated movements, balance problems, trouble walking
- Severe headaches, intense dizziness, or fainting
- Weakness, numbness, tingling, or other sensory disturbances
- Seizures (rare, but serious)
Importantly, neurotoxicity may occur:
- Alongside CRS, or
- After CRS has subsided — sometimes days later, or
- Even without any obvious prior CRS signs.
Because of this unpredictability, ongoing neurological monitoring is essential throughout therapy.
Hematologic Toxicity: Low Blood Cell Counts (Cytopenias)
Epcoritamab may suppress bone marrow or otherwise impact blood-cell production, resulting in:
- Neutropenia (low white blood cell count): increasing risk of infections
- Anemia (low red blood cells): leading to fatigue, breathlessness, pallor
- Thrombocytopenia (low platelets): increasing risk of bleeding, bruising, or poor clotting
If blood counts drop significantly:
- Even minor infections may become serious (due to neutropenia).
- Bleeding risk increases (nosebleeds, gum bleeding, easy bruising, blood in urine/stool).
- Anemia-related symptoms may worsen — affecting overall physical health.
Because of these risks, patients typically undergo blood tests before each dose, and treatment may be delayed or adjusted depending on results.
Serious Infections
Lowered immune defenses (from neutropenia, B-cell depletion, or immunomodulation) may predispose patients to:
- Respiratory infections (e.g., pneumonia)
- Urinary tract infections
- Opportunistic infections (depending on local prevalence)
- Sepsis or systemic infection — especially in severely immunocompromised individuals
Any sign of persistent fever, cough, shortness of breath, chills, severe fatigue, or unusual pain should be evaluated immediately.
Severe Allergic or Hypersensitivity Reactions
Although less common, some patients may exhibit allergic reactions during or after injection/infusion:
- Swelling of face, lips, or throat
- Hives, rash, itching
- Difficulty breathing, wheezing, or tightness in chest
- Rapid heart rate, dizziness, low blood pressure — possible anaphylactic reaction
Such symptoms demand immediate medical attention and likely halt or modify therapy.
When Epcoritamab Side Effects Usually Appear
Understanding timing helps patients and caregivers stay alert. Broadly speaking:
- First doses (especially the first full therapeutic dose): highest risk of CRS and neurologic reactions.
- During ongoing cycles (weeks to months): risks include blood count suppression (cytopenias), infections, fatigue, GI symptoms, injection-site reactions.
- Long-term or cumulative: repeated exposure may lead to chronic suppression of blood counts, recurrent infections, prolonged fatigue, or other long-term immunologic effects.
Because of this, many treatment plans call for close monitoring, especially in initial phases — including vital-sign checks, lab tests, and sometimes hospital-based observation — until patients are stable.
Why These Epcoritamab Side Effects Happen — Underlying Mechanisms
Here’s a simplified breakdown of why Epcoritamab tends to produce this variety of side effects:
- Immune overactivation → systemic inflammation (CRS): By redirecting T-cells to attack B-cells, Epcoritamab triggers immune activation. This causes elevated cytokine production, which can affect multiple organs and systems.
- Immune-mediated neurotoxicity: The same immune activation — or byproducts like cytokines — can cross into the central nervous system, disrupting neurological function.
- Bone marrow suppression or B-cell depletion → low blood counts: Whether through direct effects on immune cells or indirect immunosuppressive effects, Epcoritamab may reduce production and survival of blood cells.
- Increased infection risk: As immune cell populations drop (or immune balance is disturbed), the body’s defense against pathogens weakens.
- Local tissue reaction (from injection): The subcutaneous route may irritate skin/tissues, especially given immunogenic nature of the therapy.
- Systemic stress and organ strain: The body responding to immune activation may impose additional stress on organs, leading to fatigue, GI discomfort, or generalized symptoms.
Given these underlying causes, side effects are to be expected — but with good monitoring and supportive care, many can be managed successfully.
How to Manage & Minimize Epcoritamab Side Effects
While not all side effects can be prevented, many can be mitigated or managed. Here’s a practical guide for patients and caregivers:
1. First-Dose Monitoring & Pre-medication
- Undergo first full dose in a supervised clinical setting — often with hospital admission or monitored infusion/injection.
- Use pre-medications as prescribed (e.g., steroids, antihistamines) to reduce risk of CRS or allergic reaction.
2. Regular Lab Monitoring
- Blood counts (complete blood count — WBC, neutrophils, platelets, hemoglobin) before each dose.
- If counts are low, your doctor may delay or reduce dose, or provide supportive therapy (e.g., growth factors).
3. Report Symptoms Early — Don’t Wait
- Any fever, chills, unusual fatigue, breathing difficulty, or neurologic changes — report immediately.
- It’s better to evaluate early rather than waiting till symptoms worsen.
4. Supportive Care at Home
- Stay well-hydrated; avoid heavy meals immediately after dosing if nausea or GI upset occurs.
- Eat light, balanced meals; small frequent meals may help if appetite is poor.
- Rest adequately; avoid strenuous activity for 24–48 hours after a dose if fatigued.
- Maintain good hygiene, avoid crowded or unsanitary places to reduce infection risk.
- Use gentle skin care at injection site; avoid scratching or irritation.
5. Educate Caregivers & Family
- Inform caregivers about possible side effects and warning signs.
- Instruct them on when to get urgent care (fever, breathing difficulty, sudden weakness, bleeding).
- Keep a “therapy alert card” (if provided), showing drug name, dosing schedule, and physician contact info.
6. Plan for Follow-up & Support
- Schedule all follow-up visits and lab tests.
- Keep a symptom diary after each dose — note fever, mood, appetite, fatigue, bruising, bleeding, etc.
- Stay in contact with oncology care team — don’t hesitate to ask questions or seek help.
When to Seek Emergency Medical Help — “Red Flag” Warning Signs
If any of the following occur during or after Epcoritamab therapy, seek emergency medical attention immediately:
- High or persistent fever, uncontrolled chills, or sudden high temperature
- Shortness of breath, difficulty breathing, wheezing, or chest tightness
- Rapid or irregular heartbeat, palpitations, chest pain
- Sudden dizziness, fainting, severe weakness, or inability to stand/walk
- Confusion, slurred speech, seizures, severe headache, sudden changes in vision or coordination
- Unusual or heavy bleeding (gums, nosebleeds, blood in stool or urine), or widespread bruising
- Persistent nausea, vomiting, diarrhea, or severe abdominal pain leading to dehydration
- Signs of serious infection: high fever, chills, persistent cough, painful urination, or rapid worsening of any mild infection
Time matters — early recognition and treatment can significantly reduce risks associated with serious reactions.
Balancing Benefits vs Risks: Why Many Choose Epcoritamab
While the list of potential side effects can look daunting, for many patients, the benefits of Epcoritamab — in terms of disease control, remission potential, and improved prognosis — outweigh the risks, when managed properly. Key points:
- Epcoritamab offers a targeted immune-based approach, often effective even when other therapies have failed.
- Many side effects are manageable, with appropriate monitoring, supportive care, and timely interventions.
- As oncology care improves, supportive protocols (pre-medication, dose adjustments, monitoring) continue to evolve — improving safety outcomes.
- Patients and caregivers informed about side effects — and empowered to act quickly — can safely navigate therapy with fewer complications.
Thus, with careful planning, close communication, and medical supervision, Epcoritamab remains a valuable treatment option for eligible patients.
Final Thoughts & Practical Checklist
Epcoritamab could be a game-changer in the fight against certain B-cell lymphomas. But its power means an important responsibility for patients, caregivers, and healthcare teams.
Here’s a quick checklist to keep on hand:
✅ Make sure the first dose (or early doses) is under medical supervision
✅ Keep a schedule of lab tests and follow-up appointments
✅ Report any discomfort or unusual symptoms – the sooner the better
✅ Maintain good hygiene and a healthy lifestyle during treatment
✅ Educate caregivers and make sure they know the red-flag symptoms
✅ Get rest and support your body (hydration, nutrition, gentle activity)
✅ Communicate openly with your oncology team
With awareness, preparation, and vigilance, many patients successfully navigate epcoritamab therapy – reaping its benefits while minimizing its risks.

